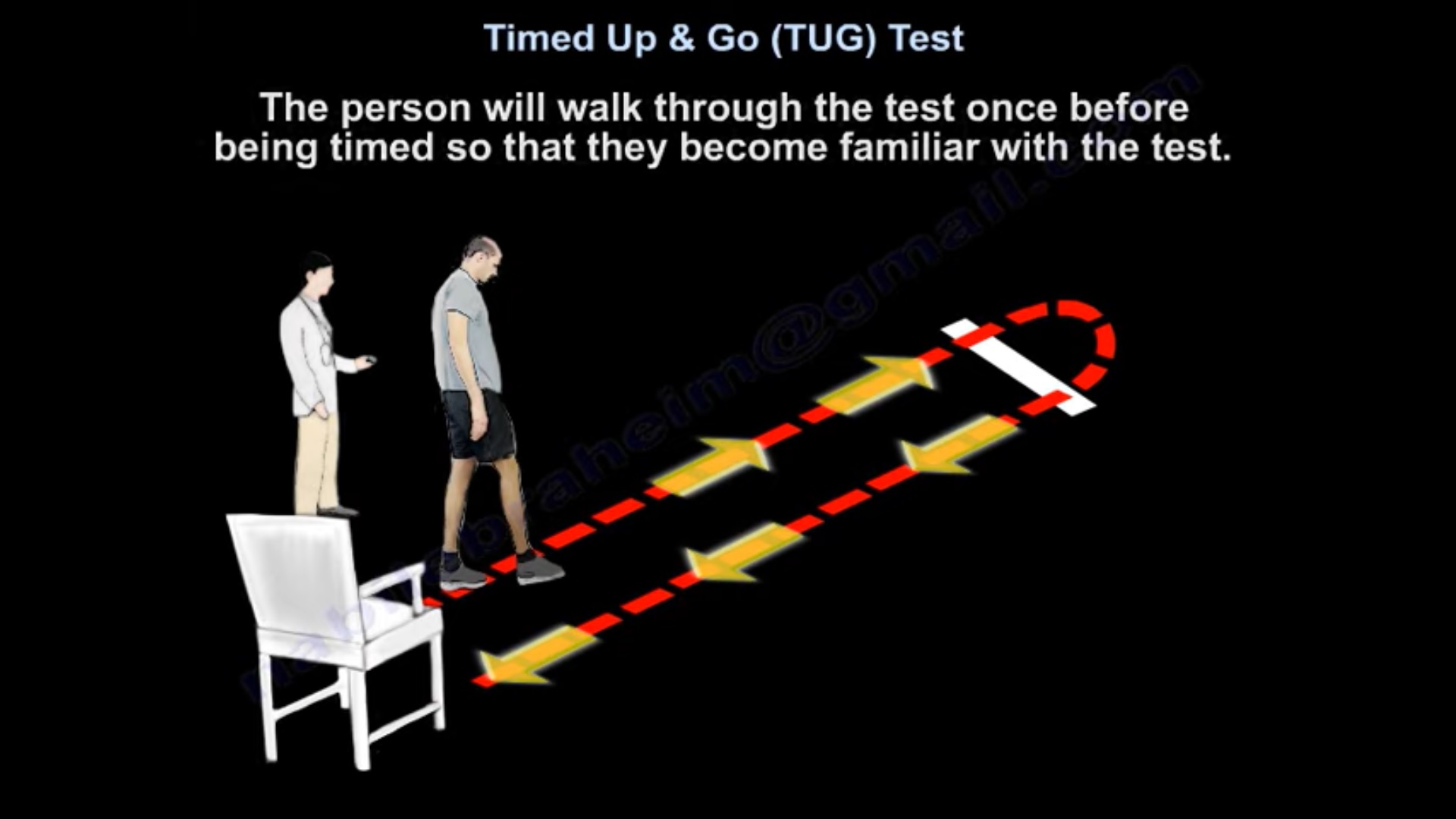
If you can’t see the link, login and then come back and the Download button will be visible.If you are logged in to, you should be able to see the link below- click to download the form. You can print it and begin using it in your department.Print Out of Test and Documentation Form Below: 2015 study by Vance et al indicated that the TUG-COG has a greater predictive value than the TUG or TUC-man for Parkinson’s patients. TUG-Cognitive (TUG-COG): Test is performed with subject counting backward by 3s from a random number while performing test. 2015 study by Tang et al indicates that TUG-man is a better indicator of pre-frailty in community dwelling adults more than 50 years old than TUG or TUG-COG. TUG-Manual (TUG-man): Test is performed with subject carrying cup of water. Pros: Valid, reliable measure of balance Recognized predictor of fall risk Correlates strongly with Berg and Functional Reach Easy to perform Quick, little space or equipment needed.Ĭons: Footgear may impact performance on test Use of assistive device and/or impaired cognition increased TUG time How Long Does It Take: 14 seconds represents increased fall risk / > 30 seconds: functional dependence The TUG uses objective timing measures, where the GUG (Get Up and Go test) assessed mobility and fall risk on a subjective scale based on rater observations and judgment. The TUG is a timed test developed by Podsiadlo and Richardson in 1991 as a modification of the GUG. What Does It Measure: The TUG is used to assess mobility, including walking speed, dynamic balance and fall risk. 
Statistically is it a “good” test - is it reliable, valid, reproducible?įor our geriatric residents, there are also multiple additional considerations including: cognition, medications and interactions, sensory impairments, endurance and the severity of the balance impairment we are attempting to measure… just to name a few.Can the test be incorporated into a treatment session?.When selecting a test to measure balance, there are multiple factors therapists consider, which ultimately help match up a test to our resident. Remember, Medicare is looking for objective clinical data– so why not give it to them!! A Quick Recap: Measuring Balance Not only that, but you will gain valuable insight into the specific limitations of your residents and be able to develop a natural progressive treatment plan to keep them on their feet! If you use an EMR, no worries, you can reference the test score in your electronic documentation and keep the paper copy in your soft chart. This objective data should be included in your clinical documentation and will support the necessity of your services and help support your goals and treatment plan. A ready-to-use printout of a customized test form that you can use in your setting immediately.The “norms” for the geriatric population.For each of the tests reviewed, we provide: Our goal with this 5-Part Blog Series is to provide the therapist working in long-term care with a series of clinically relevant objective tests and measures that can be used in your department. Just in case you missed Part 1, 2, 3 or 4, here are the links: Welcome to Part 5 – the Last of Our “Finding Your Balance” Blog Series
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
